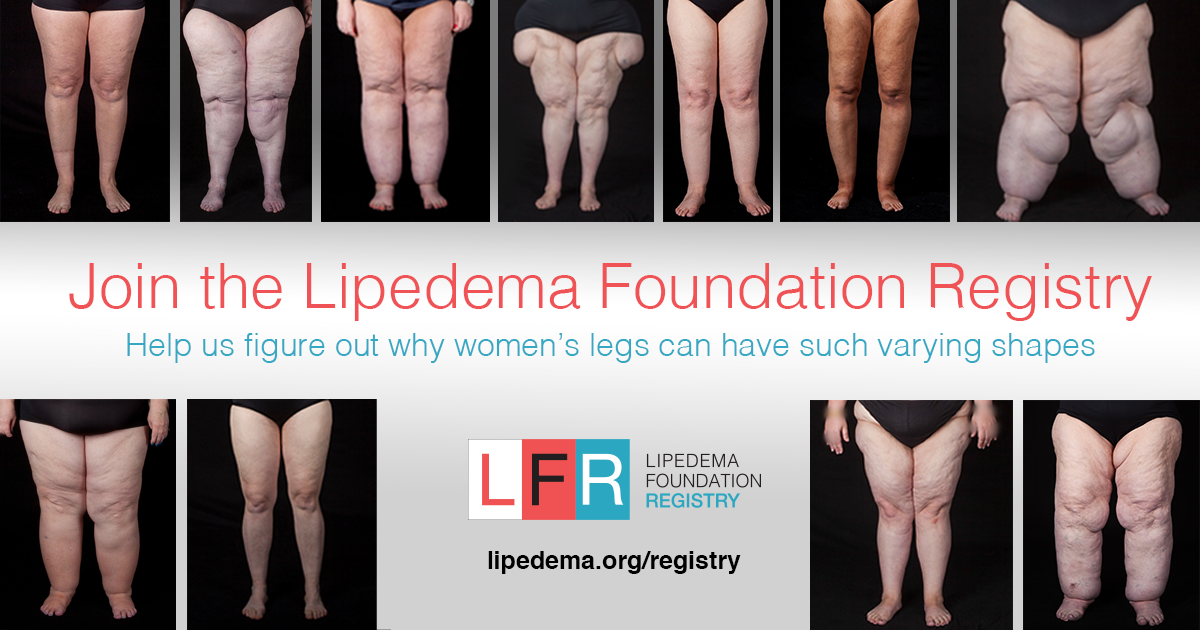
What is Lipedema?
Lipedema is a chronic medical condition that primarily affects women characterized by bilateral, symmetric buildup of adipose tissue (fat) in the legs, and sometimes the arms and lower trunk. A common but under-recognized disorder, Lipedema may cause pain, tenderness, swelling, and easy bruising. It may be accompanied by an unusual nodular and/or fibrotic texture within the fat that can feel like rice, peas, or walnuts beneath the surface of the skin. The intensity of pain may range from none to severe, and its frequency may be constant, intermittent, or only occur when the fat is palpated. Limited public awareness of Lipedema, coupled with few research-backed treatments, can lead to exacerbation of symptoms as well as physical and emotional distress.
Who Gets Lipedema?
Lipedema primarily affects females, with rare reports of development in men. Although believed to be prevalent, the exact incidence is not known.
What Causes Lipedema?
The causes of Lipedema are not well understood. It is reported to start or worsen during puberty and other periods of hormonal changes, such as pregnancy and menopause. Research is underway to determine the biological role of hormones, genetics, inflammation, and metabolism in the condition’s development.
(Read more about research direction here.)
Common Presentation / Symptoms of Lipedema
Bilateral, symmetrical buildup of fat in the legs, and sometimes arms and lower trunk, that is resistant to nutritional intervention, exercise, elevation, diuretics, and bariatric surgery
Feet/hands are typically spared, sometimes causing the appearance of an ankle or wrist “cuff”
Almost exclusively affects women
Complaints of pain, tenderness, heaviness in affected areas
Fatigue Starts or worsens at times of hormonal changes: puberty, pregnancy, or menopause
Easy bruising
Presence of nodular and/or fibrotic texture beneath the skin that can create an uneven, dimpled appearance
Edema and joint hypermobility may also be present
Helpful Resources
Among the resources throughout our website, the Lipedema Foundation maintains a Resources page where you will find everything from a Patient Self-Advocacy Guide to ICD Codes.
The Lipedema Foundation encourages you to join our Lipedema Registry, which we established to help our Lipedema community, including affected individuals, families, clinicians, and researchers.
Lipedema is not Obesity
Lipedema is distinct from obesity, although they are often confused. Obesity-related fat is different from Lipedema-related fat and occurs throughout the body. In Lipedema, the fat occurs in the limbs (and sometimes lower trunk), typically sparing the hands and feet. People with early-stage Lipedema typically do not have diabetes, high cholesterol, or high blood pressure, which are conditions that are more commonly associated with obesity.
Lipedema is not Lymphedema
The swelling in lymphedema often affects only one side of the body, and includes the hands and feet. Furthermore, lymphedema can be diagnosed with imaging or genetic tests whereas Lipedema diagnosis requires a clinical diagnosis based on patient history and physical examination.
If someone with Lipedema also has lymphatic system dysfunction, they may also present with Lymphedema. When the two conditions present together, this would be called “Lipo-lymphedema.”
Diagnosis for Lipedema
Lipedema is often misdiagnosed because it requires a clinical diagnosis by a trained clinician. Healthcare providers will evaluate a patient's history and perform a physical exam to determine a Lipedema diagnosis. There are not yet confirmatory, standardized tests, like biomarkers, blood, urine, or imaging tests.
Despite initial medical reports from more than 75 years ago, there are no definitive diagnostic tests for Lipedema. It is often misdiagnosed as obesity, lymphedema, Dercum’s disease, or chronic venous insufficiency. Comorbid Lipedema may also be present in patients with these conditions.
Currently, the only way to diagnose Lipedema is to have a trained physician perform a physical examination with a review of the patient’s medical history. See our Clinician’s Guide to Lipedema for more guidance on diagnosis. Rehabilitative therapy professionals may be confident in distinguishing Lipedema from lymphedema. Surgeons who perform liposuction are able to remove fat but may not provide broad or long-term care. According to the Lipedema Foundation First Look Report, 1/3 of participants reported their diagnosis came from a surgeon.
Quality of Life
In addition to physical symptoms, such as pain, swelling, heaviness, discomfort, and limited mobility, Lipedema can also affect an individual’s mental health and quality of life, sometimes leading to low energy, feelings of hopelessness, low self-esteem, or eating disorders. Affected individuals are encouraged to speak with their healthcare provider about their mental health. Support groups where patients can share their experiences may also be found through social media. To find these groups, go to Facebook and search Lipedema or lipoedema.
The Lipedema Foundation provides dozens of Lipedema resources to learn more.
What to Do About Lipedema
Dealing with Lipedema can be a lonely and confusing journey. Some of the primary goals of Lipedema treatment are to:
Manage Inflammation
Improve Lymphatic Flow
Reduce Fibrosis
Manage Pain
Decrease Adipose Tissue
Promote Overall Health
Prioritize Emotional and Mental Health
Increase Mobility
Minimize Fatigue
Each body is different, and no single formula works for all. People with Lipedema are encouraged to slowly incorporate different treatments into their routine to see what works best for them.
While there is currently no cure for Lipedema, there are various care and Lipedema treatment options available that can effectively manage symptoms and improve the quality of life for patients. While surgery such as liposuction can be valuable for some people to manage pain and improve mobility, the decision to undergo surgery must not be taken lightly and should be made in partnership with a qualified medical professional.
Learn more about Lipedema treatments.
Resources for Lipedema
You will find resources for Lipedema throughout our website, from our Legato Library which features all Lipedema publications, to the Research Roadmap which recommends action to grow and strengthen research in the field, to helpful guides for patients and caregivers and Lipedema treating clinicians. LF has even recently published an extensive catalog of treatment modalities and has launched a Provider Directory. The Lipedema Foundation also maintains a more general resources page where you will find things such as LF resources, published Lipedema guidelines, and patient support groups.
The Lipedema Foundation encourages you to join our Lipedema Registry, which we established to help our Lipedema community, including affected individuals, families, clinicians, and researchers.
About the Lipedema Foundation
The Lipedema Foundation aims to define, diagnose and develop treatments for Lipedema, and is the largest funder of Lipedema research. The Lipedema Foundation’s work is currently focused on better understanding and defining the biology of Lipedema, and improving the Lipedema diagnosis.
The Lipedema Foundation's website provides high-quality, medically accurate information, supported by published biomedical research and clinician and patient input. The Foundation reviews its content with a broad network of research experts, clinicians, and patient advisors.